What is Prednisolone?
Prednisolone is a corticosteroid drug used in the treatment of patients with moderate to severe rheumatoid arthritis (RA). The rationale for the use of corticosteroids in RA is the rapid control of symptoms during the phases of exacerbation of the disease mediated by the anti-inflammatory effect.
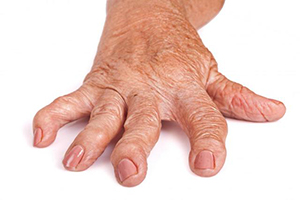
In addition to simple symptomatic improvement, corticosteroids have been shown to slow down the rate of destruction of the joints at the same like the disease-modifying antimicrobial drugs (DMARD). In current treatment strategies for less aggressive forms of AR, corticosteroids are often associated with a DMARD (usually the methotrexate that is better tolerated). Systemic side effects, even at low doses, are the main limiting factor for their long-term use. Prednisone, at a dose of 7.5 mg a day, is able to maintain good control of symptoms (which at this dose lasts only 6-12 months) and to slow the progression of joint damage to a maximum of 2-4 years without problems, after which it must be gradually reduced and suspended.
Prednisone, administered in the form of an immediate-release oral preparation, is absorbed rapidly and almost completely; reaches maximum plasma concentrations after approximately 2 hours. More than 80% of prednisone is converted into the active metabolite prednisolone via hepatic first pass metabolism. After new hepatic metabolism, prednisolone is transformed into inactive metabolites that are mainly eliminated via the kidneys. The half-life of prednisolone is about 3 hours. The profile of plasma concentrations of prednisone MRI is very similar to that of immediate-release prednisone (at the same dose) with the difference of a time to reaching delayed peak levels of about 4 hours.
MRI prednisone tablets should be taken whole around 10pm, not in the morning as is currently the case with traditional preparations. If more than 2-3 hours have passed since the evening meal, the CPR recommends taking them after a snack (eg a slice of bread with ham or cheese); fasting may reduce bioavailability.
What is Prednisolone used for?
Prednisolone is mainly used in anti-inflammatory and antiallergic therapy, in case of asthma or inflammation (arthritis). They are also used for Addison’s disease (chronic adrenocortical insufficiency characterized by hyperpigmentation, sense of weakness, weight loss, in these subjects even trivial infectious or traumatic stimuli can lead to shock), for the prevention of rejection syndrome (after transplantation of ‘organ, due to their immunosuppressive effect) and in various types of blood and skin diseases.
Like all NSAIDs, corticosteroids can also cause damage to the gastric mucosa, both by direct action and by interference with the metabolism of arachidonic acid and by decreasing the number of prostaglandins, which have a mucoprotective effect.
Other undesirable effects are:
- redistribution of body fat towards the face and neck and muscle thinning (Cushing’s syndrome)
- osteoporosis
- hyperglycemia (undesirable in diabetics) and decreased resistance to infections, which can lead to states such as oral candidiasis
- increase in wound healing time
- appearance or worsening of acne
- hirsutism effects.
They may also have mineralocorticoid effects (sodium and water retention due to aldosterone receptors binding) and blood clotting effects.
What is the difference between Prednisone and Prednisolone?
Both Prednisone and Prednisolone belong to the same class of medications called synthetic corticosteroids and are used for the treatment of the same conditions, namely ulcerative colitis and other gastro-intestinal diseases of inflammatory nature, rheumatoid diseases, airway inflammations, such as bronchitis, asthma and associated problems, etc.
Prednisone and Prednisolone are interchangeable drugs, but according to this study, the levels of Prednisolone are cleared faster and in a safer way in patients with compromised liver function, therefore its use is preferable in individuals from this subcategory.
What are the side effects of Prednisolone?
In the 3-month comparison study , there were no differences between immediate-release prednisone and MR prednisone in safety profile, but a predefined list with standardized score was not used for recording adverse events as would have been necessary. In the open-label extension study, with a median duration of treatment of 281 days and a mean prednisone dose of 6.8 mg per day, the incidence of adverse events was 51% (including a 4.8 % drop out), similar to that of historical controls.
During the 12 months of observation required by the controlled study and by the open-label extension phase, the corticotropin release hormone (CRH) response test performed in three steps several (at the baseline, at the end of the 3 months in double blind and 9 months in the open) on a small group of patients (n = 28) did not find signs of suppression of the pituitary-adrenal axis.
Precautions
A single dose of cortisonic, even very high, is practically devoid of toxic effects, which occur with the chronicity of the use of the drug. The main problem that can lead to prolonged use of these drugs is adrenal insufficiency, which can also become fatal.
Contraindications
 Prolonged therapy should be interrupted gradually; corticosteroids are contraindicated in cases of:
Prolonged therapy should be interrupted gradually; corticosteroids are contraindicated in cases of:
- ulcer
- diabetes
- heart failure
- osteoporosis
- hypertension
Where can you buy Prednisolone online?
 Prednisolone is a generic version of more expensive brand medications containing the same active component. Generic drugs are easily available online, but caution should be exercised when ordering healthcare products. Find a vendor with clearly formulated terms and conditions of use, as well as protected customer privacy and secure payment. A good online pharmacy makes buyer’s health its priority, so look for e-drugstores where healthcare services are included or offered as an option.
Prednisolone is a generic version of more expensive brand medications containing the same active component. Generic drugs are easily available online, but caution should be exercised when ordering healthcare products. Find a vendor with clearly formulated terms and conditions of use, as well as protected customer privacy and secure payment. A good online pharmacy makes buyer’s health its priority, so look for e-drugstores where healthcare services are included or offered as an option.
One can buy Prednisolone online and have it delivered to a specified address. This convenience does not exempt you from your responsibility as a patient: you need to be aware of existing contraindications and possible pharmacological interactions to avoid. Medical consultation is required under all circumstances.
What are other names for Prednisolone?
- Aripride – Sarian Healthcare
- Depotex – German Remedies (Aeroforce)
- Emcort – Captab Biotec
- Intralone – Intra Labs India Pvt. Ltd.
- Lumi-M – Aronex Lifesciences Pvt. Ltd.
- Macpred – Macleods Pharmaceuticals Ltd. (Macphar)
- Nicort – AHPL
- Paxopred – Pax Healthcare
- Predace – Micro Labs Ltd (Gratia)
- Predon-M – Orion Biotech Pvt. Ltd.
- Predzest Tablet – Innovative Pharmaceuticals
- Predzen Tablet – Ikon Remedies Pvt. Ltd.
- Premisol – Molekule India Pvt. Ltd.
- Zencort-M – Zenon Healthcare Ltd
Posted in Anti-Inflammatory
(3 voices, average: 5 of 5) 28241 views