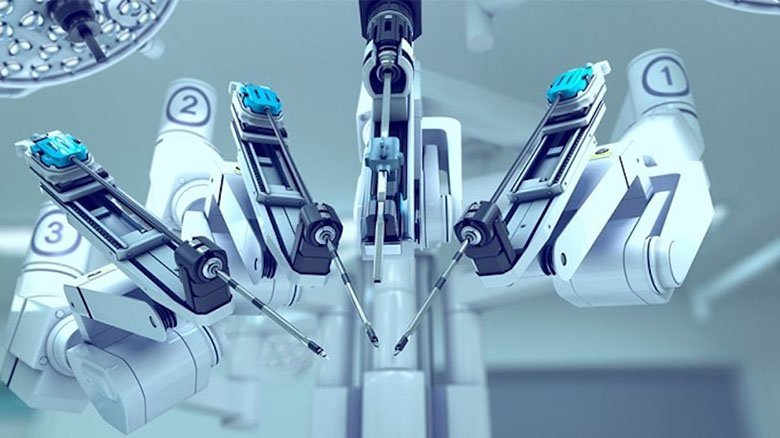
The future has already come to healthcare and it goes on developing. A robot in the operation-room is already not surprising in many hospitals. The use of these extremely accurate machines makes it possible to minimize the risks for a doctor to make a mistake and for a patient to come through the operation with complications.
Robots became not only a part of the operational equipment, but they are also widely used in distant diagnostics, rehabilitation, and taking care of the patients staying in hospitals.
Surgical robots
One of the best examples of robotics application in medicine is surgical robots. Thanks to these machines, surgeons can perform the manipulations with extreme accuracy. Such robots are commonly used in laparoscopic and minimally invasive operations, which give the possibility to make the patient’s postoperative period much easier and reduce the time for complete recovery.
Rehabilitation robots
Numerous researches on using robots for the rehabilitation of physically disabled people give hope for hundreds of thousands of people who have overlived strokes, got serious injuries in car accidents or got traumatized in some other situation and lost their ability to move.
Bionic extremities, for example, have already been successfully used in people who needed a prosthesis. Due to such technologies, they’ve got the possibility not only to eliminate an aesthetic defect but also get a comparatively functional hand or leg.
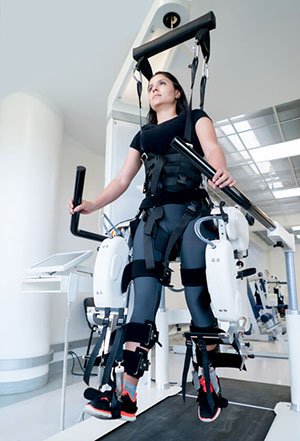
Another recent development of robotics in healthcare is an exoskeleton. Using the signals sent from the brain, it can help people who have been paralyzed or move with the help of wheelchairs to sit, stand, and even walk. Even though this technology is still being developed and is not yet available for everyone who needs it, the scientists are on the right track.
Robotics in the healthcare is progressing day by day and, who knows, maybe tomorrow we’ll be able to witness an invention of a new robot that will change our usual understanding of medicine.